I hear it all. As the CEO of the National Community Pharmacists Association (NCPA), I have the awesome opportunity to speak in-person to over 5,000 pharmacy owners most years − the very people the organization exists to represent. During those conversations, owners usually have two issues on their minds: here and now issues (keeping the lights on per se) and where the profession is going in the future (seeing around the corner).
There’s no shortage of here and now issues. Direct and Indirect Remuneration (DIR) fees are at the top of the list. Slow and low Maximum Allowable Cost (MAC) is right there too, as well as allowing consumers’ pharmacy choice. Spreading the word that Pharmacy Benefit Managers (PBMs) contribute to the higher costs of prescription drugs rather than reduce them is important. Heavy-handed Food and Drug Administration (FDA) enforcement on compounding is yet another.
Here and Now Challenges Include PBMs
Believe it or not, PBMs actually serve a function. If they didn’t exist, some entity would put together a network of pharmacies. Someone would negotiate formularies with pharmaceutical manufacturers and someone would process claims.
Unfortunately, PBMs have morphed into something that takes advantage of the very customers they were created to serve. For a long time, it was just pharmacies receiving the short end of the stick. However, now PBMs are biting the very hand of all of those that feed them: pharmacies, pharmaceutical manufacturers, plan sponsors/payers and even consumers. All are being forced to feed them a steady diet of dollars.
Pharmacy school was hard enough. Trying to explain our courses to non-science students was sometimes even harder. Fast forward past graduation and consider how difficult it is to explain the ins and outs of PBM practices to patients and lawmakers.
Why try? Because we need them on our side if we are going to make progress in changing the PBM model. If non-pharmacists are to help us, they need a general understanding of what PBMs do and how they got here. That understanding must supersede that little Rx drug card in their wallet or purse.
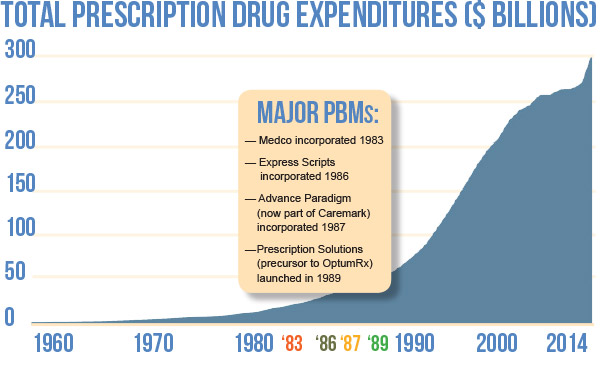 There is plenty of information that indicts PBMs. One of the most telling is to look at what has happened to expenditures on drugs since PBMs were incorporated in the mid-80s. PBMs have built their reputation on controlling costs.
There is plenty of information that indicts PBMs. One of the most telling is to look at what has happened to expenditures on drugs since PBMs were incorporated in the mid-80s. PBMs have built their reputation on controlling costs.
To the contrary, the data shows that prescription drug expenditures have gone up 1,010 percent since 1987! During the same period, overall price inflation has only gone up 125.9 percent (not exactly the Merriam-Webster definition of control).1
PBMs are also a phenomenon unique to our country. Talk with pharmacists from other countries, and they will have little or no awareness about what a PBM is or does. Yet, even
though Americans have the benefit of PBMs protecting their drug costs, the U.S. pays far more than any other country for prescription drugs.
It can be complicated, but the NCPA has simplified the PBM story with a booklet and video that can be shared with your legislators, the media and your customers who are responsible for the financials of your local employers. It’s called The PBM Story: What They Say, What They Do, and What Can Be Done About It.
 The booklet is now available for download in either a six-page or 12-page format at https://www.ncpanet.org/advocacy/pbm-storybook.
The booklet is now available for download in either a six-page or 12-page format at https://www.ncpanet.org/advocacy/pbm-storybook.
Some of your patients and lawmakers don’t want to know how the clock was made; they just want to know what time it is. That’s what The PBM Story does.
Where Change Begins
Change starts with strengthening federal regulations that govern PBMs by enacting pro-patient, pro-pharmacy bills in Congress. The following must be on the list: banning retroactive pharmacy DIR fees (S. 413/H.R.1038), sharing the role that PBMs play in increasing drug costs with opinion leaders and unchaining the abilities of community pharmacies to help lower overall healthcare costs.
Positioning for the Future
You can guarantee your big chain competitors are paying millions for insight (seeing around the corner) to help them forecast the right moves for their businesses. NCPA membership is an inexpensive way to get market insight to help you make strategic decisions to keep your business strong and relevant.
Enhanced Services
- Home Delivery
- Adherence Packaging
- Medication Synchronization
- Medication Therapy Management (MTM)/Comprehensive Medication Review (CMR)
Hopefully, all or most of these services are already familiar to your pharmacy. Now, answer these two questions:
Do your big box chain competitors provide these services?
When a patient receives these services at your pharmacy rather than at the big box chains, do you get paid more than they do?
There’s a great chance you answered “no” to both questions. That’s the current situation for community pharmacies, and it doesn’t make sense. It’s like Volkswagen charging the same price for a Jetta as they do for a Lamborghini (Volkswagen Group owns Lamborghini). Both are cars with four wheels and a steering wheel that transport passengers. But the driver experience between the two is radically different! No one would expect to pay the same amount for both cars. So, why are community pharmacies providing more services for the same cost as their chain counterparts?
The time has come when the enhanced services we mostly give away are recognized as valuable. Local enhanced services networks providing services (some listed previously) valued by payers to help lower overall healthcare costs have developed in more than 20 states. These networks differentiate the average pharmacy experience from those pharmacies that produce greater health and economic outcomes. Some payers may even give networks of pharmacies preference to dispense prescriptions if they show they can solve other problems like patient adherence, medication access through true home delivery or improved transitions of care from hospitals to the community.
Why Join a Network?
There is a terrific video called “Breaking Down Walls” at www.cpesn.com/why-join/. It’s about 11 minutes. If you don’t have that much time to spare, watch just a few minutes of it and see if you agree with the concept. If you do, position your pharmacy to be part of a local enhanced services network. Chances are someone in your state is already working on such a network. Join them.
Among its many offerings, the 2017 NCPA Annual Meeting, October 14-17, will feature a number of sessions on enhanced pharmacy service networks. There will be pharmacy owners who have contracts with payers sharing their experiences, as well as pharmacy owners who are just getting started or just wanting to figure out what this movement is all about. To register, call 800.544.7447 or visit www.ncpanet.org/meetings/annual-convention.
Whether you are thinking about the here and now or what’s around the corner, NCPA has a strategy. With your active participation, community pharmacy has a bright and viable future.
Source:
1 Centers for Medicare & Medicaid Services, Office of the Actuary, National Health Statistics Group.

Comments (0)